Integrative Breast Cancer Support
By Remi Odisho
How Nutrition and Acupuncture Can Improve Side Effects, Recovery, and Quality of Life
A breast cancer diagnosis brings not only complex medical decisions, but also a significant physical and emotional burden. Treatments such as chemotherapy, radiation, and endocrine therapies including tamoxifen and aromatase inhibitors (AIs) are essential components of care, yet they often come with a wide range of side effects that can impact day-to-day functioning and long-term wellbeing.
Integrative oncology focuses on supporting the body alongside these treatments — not as an alternative, but as a way to improve tolerance, reduce side effects, and enhance recovery. Two of the most valuable and evidence-informed tools in this space are targeted nutrition and acupuncture, both of which are supported in clinical guidelines for breast cancer care (Greenlee et al., 2017; Lyman et al., 2018).
Why Integrative Support Is Essential During Breast Cancer Treatment
Cancer treatment places the body under sustained physiological stress. Chemotherapy, for example, targets rapidly dividing cells, which includes not only cancer cells but also healthy cells in the gut and mucosal lining, hair follicles, bone marrow and immune system. Endocrine therapies such as tamoxifen and aromatase inhibitors alter oestrogen signalling, which can have downstream effects on joints, mood, sleep, and metabolic health.
These treatments are life-saving, however they can also disrupt key systems involved in resilience — including the nervous system, digestive system, and hormonal pathways.
This is where integrative support becomes critical. By addressing these systems proactively, we can often reduce the severity of side effects, support patients to remain consistent with their prescribed treatments and ultimately maintain quality of life during, and after, treatment, (Greenlee et al., 2017).

Nutrition During Breast Cancer Treatment: Supporting the Body Under Stress
Nutrition in the context of breast cancer is not about restriction or rigid protocols. Instead, it is about providing the body with the nutrients it needs to repair, regulate inflammation, and maintain energy during a time of increased demand.
Chemotherapy and radiation can increase oxidative stress and inflammation within the body. Thus, nutrient-dense foods rich in antioxidants, polyphenols, and essential fatty acids help modulate this response, supporting cellular repair while also protecting healthy tissue, (Rock et al., 2020).
Adequate protein intake is particularly important during treatment. Protein provides the building blocks required for tissue repair, immune function, and maintaining muscle mass, which is often compromised during periods of fatigue and reduced activity, (Rock et al., 2020).
At the same time, treatment-related side effects such as nausea, taste changes, and reduced appetite can make eating more challenging. A personalised approach to nutrition helps patients maintain adequate intake in a way that feels achievable, rather than overwhelming.
Managing Side Effects Through Targeted Nutritional Support
Many of the most common side effects of breast cancer treatment are closely linked to changes in the gastrointestinal system and inflammatory pathways.
For example, chemotherapy can disrupt the rapidly dividing cells of the gut lining, leading to symptoms such as nausea, diarrhoea, constipation, and reduced nutrient absorption. Strategic nutritional support can help stabilise digestion, reduce irritation, and maintain hydration and electrolyte balance, (van Vliet et al., 2010).
Blood sugar regulation is another important factor. Fluctuating blood glucose levels become difficult to regulate in response to inflammation which can worsen fatigue, irritability, and cravings, particularly when appetite is inconsistent. Regular, balanced meals that include protein, complex carbohydrates, fibre, and healthy fats can help stabilise energy levels throughout the day.
Rather than applying a one-size-fits-all diet, integrative nutrition focuses on adapting food choices to the patient’s current symptoms, treatment stage, and tolerance.
Gut Health, the Microbiome, and Breast Cancer Recovery
The gut plays a central role in both short-term treatment tolerance and long-term recovery.
The gut microbiome influences immune function, inflammation, and even how oestrogen is metabolised and cleared from the body. This is particularly relevant in hormone receptor-positive breast cancer, where oestrogen balance remains an important consideration even after active treatment has finished, (Plottel & Blaser, 2011; Kwa et al., 2016).
Chemotherapy, medications, and stress can all disrupt microbial diversity and gut barrier integrity. This can contribute to ongoing fatigue, digestive symptoms, hormonal dysregulation and increased systemic inflammation.
Supporting gut health through nutrition helps restore microbial balance, improve nutrient absorption, and support detoxification pathways involved in hormone metabolism. Over time, this can have a meaningful impact on both symptom burden and overall resilience.

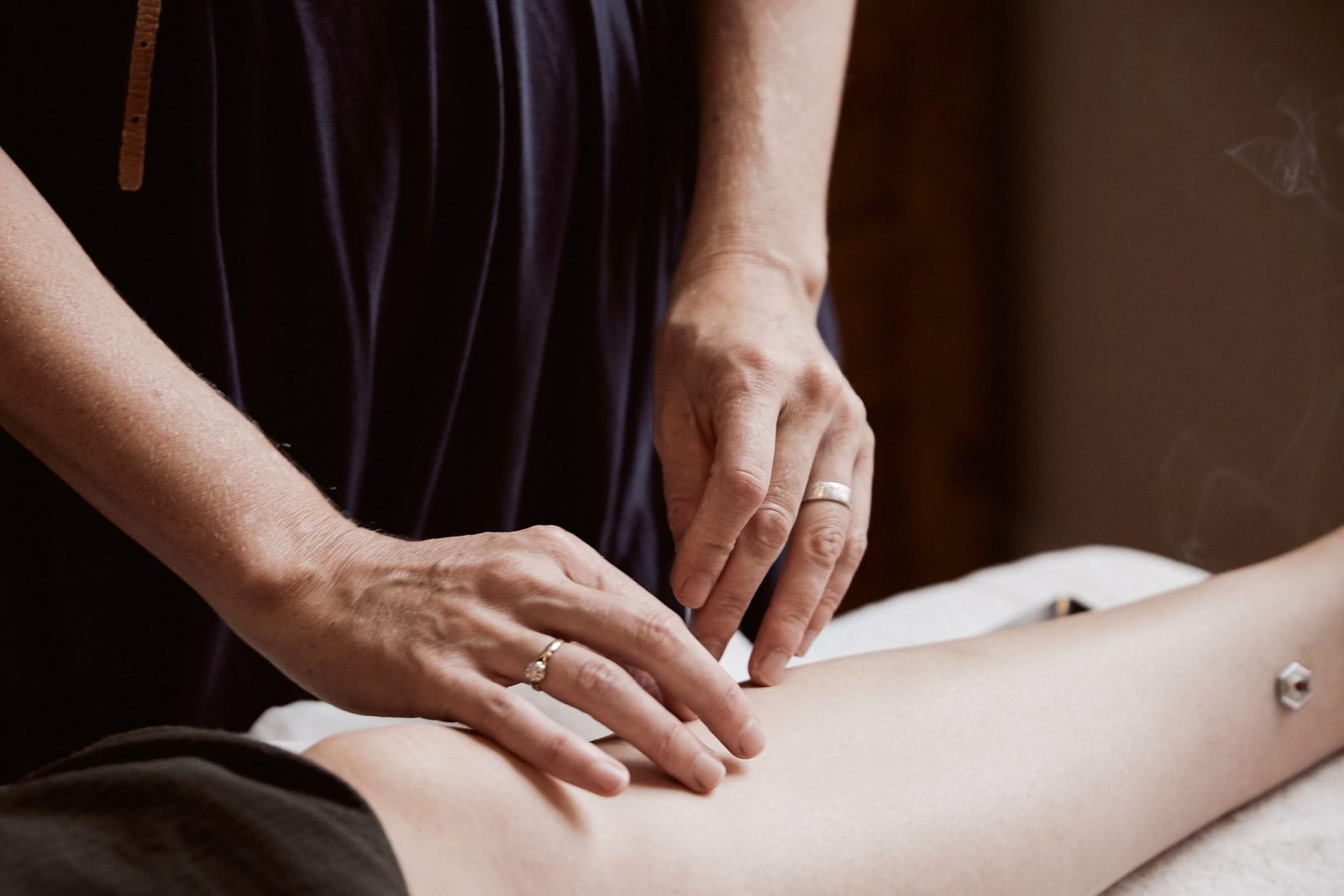
Acupuncture in Breast Cancer Care: Mechanisms and Clinical Benefits
Acupuncture is increasingly integrated into oncology care due to its ability to modulate multiple physiological systems simultaneously.
From a biomedical perspective, acupuncture influences the central nervous system, autonomic nervous system, and neuroendocrine pathways. It has been shown to affect neurotransmitters such as serotonin and endorphins, regulate inflammatory markers (specifically, TNF and IL-6), and modulate pain signalling pathways, (Garcia et al., 2013; Li et al., 2021).
This is why acupuncture can be helpful across a wide range of symptoms experienced during breast cancer treatment, including nausea, fatigue, peripheral neuropathy, hot flushes, and joint pain associated with endocrine therapies, (Chiu et al., 2016; Lu et al., 2016).
Supporting Side Effects of Tamoxifen and Aromatase Inhibitors
For many patients, the transition from active treatment into endocrine therapy presents a new set of challenges. Medications such as tamoxifen and aromatase inhibitors are designed to reduce oestrogen activity, but this can also lead to side effects including joint pain, stiffness, hot flushes, mood changes, and sleep disruption.
Acupuncture has been shown to support vasomotor symptoms such as hot flushes by influencing thermoregulatory centres in the brain. It can also help reduce joint pain and stiffness through its effects on inflammation and circulation, (Hershman et al., 2018; Chien et al., 2017).
Importantly, by improving symptom management, integrative support may help patients remain consistent with their prescribed medications — which is critical for long-term outcomes.
Stress, Nervous System Regulation, and Emotional Wellbeing
A cancer diagnosis is not only a physical experience, but also a deeply emotional one. Chronic stress can affect immune function, sleep, digestion, and hormone regulation — all of which are already under strain during treatment.
Psychophysiological stress has been shown to influence cancer-related fatigue, immune response, and overall quality of life (Bower, 2014). Supporting the nervous system is therefore a key component of integrative care.
Acupuncture helps shift the body from a sympathetic (“fight or flight”) state into a parasympathetic (“rest and repair”) state, supporting emotional regulation and resilience (Antoni et al., 2006).
Sleep as a Foundation for Recovery
Sleep is one of the most important — and often most disrupted — aspects of breast cancer care.
Treatment side effects, anxiety, and hormonal therapies can all interfere with sleep quality. Poor sleep has been associated with increased fatigue, reduced immune function, and poorer overall outcomes in patients with cancer, (Irwin, 2013; Garland et al., 2014).
Both nutrition and acupuncture can support sleep by stabilising blood sugar, supporting neurotransmitter production, and calming the nervous system. Over time, improving sleep quality can have a ripple effect across many other symptoms.
Beyond Treatment: Supporting Recovery and Survivorship
The end of active treatment is often expected to bring relief, yet many patients continue to experience fatigue, anxiety, hormonal symptoms, digestive issues, and a sense of disconnection from their previous level of health.
This phase of survivorship is a critical opportunity to rebuild.
Integrative care during this time focuses on restoring energy, supporting metabolic and hormonal balance, reducing inflammation, and improving overall quality of life. By addressing the underlying systems affected during treatment, patients can move beyond simply “getting through” cancer and begin to feel like themselves again.
A Personalised Approach to Integrative Breast Cancer Support
There is no single protocol that suits every patient. The most effective integrative care is tailored to the individual, taking into account their diagnosis, treatment plan, symptom profile, nutritional status, and personal goals.
This approach allows for targeted, meaningful interventions rather than overwhelming or unnecessary recommendations.
If you are currently undergoing breast cancer treatment or navigating life after treatment, I offer integrative support designed to work alongside your medical care.
My approach includes personalised nutrition, acupuncture for symptom management, and targeted support for fatigue, gut health, sleep, and hormonal side effects related to treatments such as chemotherapy, tamoxifen, and aromatase inhibitors.

By Remi Odisho
About the Author
Remi Odisho is an integrative naturopath and acupuncturist with a special interest in female reproductive health, digestion, hormones, and midlife transitions. Remi supports women through breast cancer treatment using evidence-based functional testing, personalised nutrition, lifestyle medicine, and integrative therapies to reduce treatment side effects and enhance recovery after treatment. Their approach is holistic, compassionate, and grounded in helping women feel informed, empowered, and supported through every stage of treatment.





